|
Overview
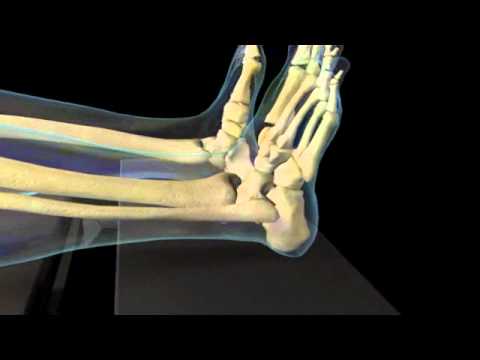 Flat feet (also called pes planus or fallen arches) is a postural deformity in which the arch of the foot collapses, with the entire sole of the foot coming into complete or near-complete contact with the ground. Some individuals (an estimated 20-30% of the general population) have an arch that simply never develops in one foot (unilaterally) or both feet (bilaterally). Causes Most cases of flatfeet are simply the result of normal development. When that is not the case, the condition can be caused by a number of factors, including the following, Age, disease, injury, obesity or being overweight, physical abnormality, pregnancy. Flattened arches in adults may result from the stresses of aging, weight gain, and the temporary increase in elastin (protein in connective tissue) due to pregnancy. In some cases, flatfeet are caused by a physical abnormality, such as tarsal coalition (two or more bones in the foot that have grown together) or accessory navicular (an extra bone along the side of the foot). The effects of diseases such as diabetes and rheumatoid arthritis can lead to flatfeet. An injury (e.g., bone fracture, dislocation, sprain or tear in any of the tendons and ligaments in the foot and leg) also can cause flatfeet. Symptoms Structural problems in your feet like fallen arches can alter your walking pattern, running pattern and cause pain throughout your body. Clear and accurate assessment of the mechanics of your lower limbs is key to understanding the profound effect that subtle faults in your foot, ankle, knee and hip alignment can cause. Diagnosis If you notice that your feet are flat, but you?re not really experiencing any pain, then you?re probably okay to go without a visit to the podiatrist (unless, of course, you have a lack of feeling in your foot). You can schedule a hair appointment instead, or maybe see a movie. However, once painful symptoms start to appear, it?s better to skip the hirsute (or cinematic) experience and go see your foot doctor. Your podiatrist will likely make the diagnosis by examining your foot visually, asking about symptoms you may be experiencing, and may test your muscle strength. You may be asked to stand on your toes (in a ballerina pose, if you prefer, although that?s certainly not required), or walk around the examining room, and you may need to show the podiatrist your shoes. He or she may comment on your excellent taste in footwear, but is more likely to check your shoes for signs of wear that may indicate fallen arches. Your podiatrist may recommend X-rays, a CT scan or an MRI in order to get a look at the interior of your foot, although the best diagnosis usually comes from the doctor?s own in-person examination. pes planus radiology Non Surgical Treatment Foot orthotic devices can stabilize some of the causes of flat feet, optimize muscle function and reduce the occurrence of painful symptoms. Generally, a custom-made semi-rigid functional posted orthotic is effective for flat feet. These devices are prescribed based on a thorough biomechanical examination by a qualified chiropodist/podiatrist. Over-the-counter arch supports may be helpful for mild cases, but often prove ineffective to relieve symptoms associated with flatfoot. Wear shoes with a good fit in the arch. Keep active and fit to strengthen leg and foot musculature. Control body weight to decrease load on the feet. Avoid prolonged periods weight bearing with bare feet. Taping to support strained ligaments and joints. Physical therapy modalities such as ultrasound. Referral for surgical correction a severe symptomatic flatfoot. Surgical Treatment  Surgery for flat feet is separated into three kinds: soft tissue procedures, bone cuts, and bone fusions. Depending on the severity of the flat foot, a person?s age, and whether or not the foot is stiff determines just how the foot can be fixed. In most cases a combination of procedures are performed. With flexible flat feet, surgery is geared at maintaining the motion of the foot and recreating the arch. Commonly this may involve tendon repairs along the inside of the foot to reinforce the main tendon that lifts the arch. When the bone collapse is significant, bone procedures are included to physically rebuild the arch, and realign the heel. The presence of bunions with flat feet is often contributing to the collapse and in most situations requires correction. With rigid flat feet, surgery is focused on restoring the shape of the foot through procedures that eliminate motion. In this case, motion does not exist pre-operatively, so realigning the foot is of utmost importance. The exception, are rigid flat feet due to tarsal coalition (fused segment of bone) in the back of the foot where freeing the blockage can restore function. After Care Time off work depends on the type of work as well as the surgical procedures performed. . A patient will be required to be non-weight bearing in a cast or splint and use crutches for four to twelve weeks. Usually a patient can return to work in one to two weeks if they are able to work while seated. If a person's job requires standing and walking, return to work may take several weeks. Complete recovery may take six months to a full year. Complications can occur as with all surgeries, but are minimized by strictly following your surgeon's post-operative instructions. The main complications include infection, bone that is slow to heal or does not heal, progression or reoccurrence of deformity, a stiff foot, and the need for further surgery. Many of the above complications can be avoided by only putting weight on the operative foot when allowed by your surgeon.
0 Comments
Overview
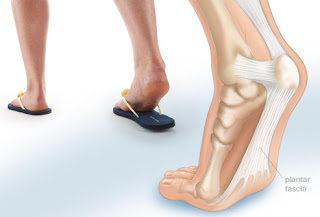 Every mile you walk puts tons of stress on each foot. Your feet can handle a heavy load, but too much stress pushes them over their limits. When you pound your feet on hard surfaces playing sports or wear shoes that irritate sensitive tissues, you may develop heel pain, the most common problem affecting the foot and ankle. A sore heel will usually get better on its own without surgery if you give it enough rest. However, many people ignore the early signs of heel pain and keep on doing the activities that caused it. When you continue to walk on a sore heel, it will only get worse and could become a chronic condition leading to more problems. Causes In our pursuit of healthy bodies, pain can be an enemy. In some instances, however, it is of biological benefit. Pain that occurs right after an injury or early in an illness may play a protective role, often warning us about the damage we've suffered. When we sprain an ankle, for example, the pain warns us that the ligament and soft tissues may be frayed and bruised, and that further activity may cause additional injury. Pain, such as may occur in our heels, also alerts us to seek medical attention. This alert is of utmost importance because of the many afflictions that contribute to heel pain. Symptoms Both heel pain and heel spurs are frequently associated with an inflammation of the long band of tissue that connects the heel and the ball of the foot. The inflammation of this arch area is called plantar fasciitis. The inflammation maybe aggravated by shoes that lack appropriate support and by the chronic irritation that sometimes accompanies an athletic lifestyle. Achilles Tendinopathy, Pain and inflammation of the tendon at the back of the heel that connects the calf muscle to the foot. Sever?s, Often found in children between the ages of 8 - 13 years and is an inflammation of the calcaneal epiphyseal plate (growth plate) in the back of the heel. Bursitis, An inflamed bursa is a small irritated sack of fluid at the back of the heel. Other types of heel pain include soft tissue growths, Haglunds deformity (bone enlargement at the back of the heel), bruises or stress fractures and possible nerve entrapment. Diagnosis A podiatrist (doctor who specializes in the evaluation and treatment of foot diseases) will carry out a physical examination, and ask pertinent questions about the pain. The doctor will also ask the patient how much walking and standing the patient does, what type of footwear is worn, and details of the his/her medical history. Often this is enough to make a diagnosis. Sometimes further diagnostic tests are needed, such as blood tests and imaging scans. Non Surgical Treatment Calf stretch, Heel cups/lifts, ice, night splint, physical therapy, activity modification. Sometimes immobilization in a cast or boot may be necessary. Topical creams, such as Voltaren or Ketoprofen, have been found to have some benefit. In some cases, the tendon may become degenerative (tendonosis). In these instances, treatment is more difficult. Prolonged periods of immobilization and physical therapy may be required. In resistant cases, surgical debridement of the tendon may be necessary. Rarely does a symptomatic achilles tendon rupture. Most achilles ruptures are not associated with prodromal symptoms. Achilles ruptures are more common in men and "weekend warriors," ie middle aged men who like to play sports (soccer, softball, basketball) on the weekends. Surgical Treatment When a diagnosis of plantar fasciitis is made early, most patients respond to conservative treatment and don?t require surgical intervention. Often, when there is a secondary diagnosis contributing to your pain, such as an entrapped nerve, and you are non-responsive to conservative care, surgery may be considered. Dr. Talarico will discuss all options and which approach would be the most beneficial for your condition. deelsonheels Prevention  Heel pain is commonly caused from shoes that do not fit properly. In addition, shoes need to have ample cushioning and support, particularly through the heel, ball of the foot, and arch. Shoes should also be replaced if they become too worn. One sure sign of wear and tear is overly worn areas of a shoe's insoles. If the heel or ball of the foot is particularly worn, damage could easily occur since the bottom of the foot is not getting the cushioning it needs. Overview
Leg length difference (LLD) is primarily when the hips are not level, causing a limp from side to side. Most practitioners divide LLD into anatomical or functional. Anatomical is when there is a true difference in the length of the tibia/fibula or the femur bone, or both. While functional LLD are either the shortening or lengthening of a limb, secondary to joint contracture or muscle imbalances.  Causes Some limb-length differences are caused by actual anatomic differences from one side to the other (referred to as structural causes). The femur is longer (or shorter) or the cartilage between the femur and tibia is thicker (or thinner) on one side. There could be actual deformities in one femur or hip joint contributing to leg length differences from side to side. Even a small structural difference can amount to significant changes in the anatomy of the limb. A past history of leg fracture, developmental hip dysplasia, slipped capital femoral epiphysis (SCFE), short neck of the femur, or coxa vara can also lead to placement of the femoral head in the hip socket that is offset. The end-result can be a limb-length difference and early degenerative arthritis of the hip. Symptoms As patients develop LLD, they will naturally and even unknowingly attempt to compensate for the difference between their two legs by either bending the longer leg excessively or standing on the toes of the short leg. When walking, they are forced to step down on one side and thrust upwards on the other side, which leads to a gait pattern with an abnormal up and down motion. For many patients, especially adolescents, the appearance of their gait may be more personally troublesome than any symptoms that arise or any true functional deficiency. Over time, standing on one's toes can create a contracture at the ankle, in which the calf muscle becomes abnormally contracted, a condition that can help an LLD patient with walking, but may later require surgical repair. If substantial enough, LLD left untreated can contribute to other serious orthopaedic problems, such as degenerative arthritis, scoliosis, or lower back pain. However, with proper treatment, children with leg length discrepancy generally do quite well, without lingering functional or cosmetic deficiencies. Diagnosis The only way to decipher between anatomical and functional leg length inequalities (you can have both) is by a physical measurement and series of biomechanical tests. It is actually a simple process and gets to the true cause of some runner?s chronic foot, knee, hip and back pain. After the muscles are tested and the legs are measured it may be necessary to get a special X-ray that measures both of your thighs (Femurs) and legs (Tibias). The X-ray is read by a medical radiologist who provides a report of the actual difference down to the micrometer leaving zero room for error. Once the difference in leg length is known, the solution becomes clear. Non Surgical Treatment Treatment for an LLD depends on the amount of difference and the cause, if known. The doctor will discuss treatment options carefully with you and your child before any decisions are made. It is important to note that treatment is planned with the child?s final height and leg lengths in mind, not the current leg lengths. Treatment is generally not needed if the child?s final LLD is predicted to be 2 centimeters or less at full height. However, the child should return to an orthopaedic doctor by age 10 for re-evaluation. Treatment is often recommended for LLDs predicted to be more than 2 centimeters at full height. If treatment is done, it usually doesn?t begin until the child starts walking. Possible treatment options include, A ?lift? in one shoe to level the child?s hips. This is often the only treatment needed for small discrepancies.  deelsonheels Surgical Treatment Surgeries for LLD are designed to do one of three general things ? shorten the long leg, stop or slow the growth of the longer or more rapidly growing leg, or lengthen the short leg. Stopping the growth of the longer leg is the most commonly utilized of the three approaches and involves an operation known as an epiphysiodesis , in which the growth plate of either the lower femur or upper tibia is visualized in the operating room using fluoroscopy (a type of real-time radiographic imaging) and ablated , which involves drilling into the region several times, such that the tissue is no longer capable of bone growth. Because the epiphyseal growth capabilities cannot be restored following the surgery, proper timing is crucial. Usually the operation is planned for the last 2 to 3 years of growth and has excellent results, with children leaving the hospital within a few days with good mobility. However, it is only appropriate for LLD of under 5cm. Overview
In medical terms, a bunion, or hallux valgus, is a bony bump that forms around the joint at the base of your big toe. This joint is one of the most important parts of your foot, bearing most of your body weight. The bony bump is caused by the head of the first metatarsal bone (the long bone) behind the big toe angling out from the foot. This causes the joint to swell, pushing the big toe in towards the adjacent toes. The result is pain on the side of your foot, arch pain, and discomfort throughout the adjacent toes as well. Causes Bunions are a common problem that can cause foot pain and difficulty wearing shoes. Bunions occur in about 30% of the population of most Western countries. They are seen most commonly in women and become more common as people get older. Patients with bunions generally have one of two problems that can cause pain. As the big toe becomes more and more angled (pointing toward the other toes), the base of the toe becomes more and more prominent, forming the bunion. The bunion forms in part because of the new angle of the toe, and in part due to inflammation over the bunion surface. As the inflammation worsens, people can experience pain with shoe wear and walking. The big toe may eventually come to lie over, or more commonly under, the second toe. This may cause further irritation while wearing shoes and more pain. The second toe of patients who have bunions commonly forms a hammer toe. SymptomsPain in the toe joint and surrounding area. Painful to touch or press, and when walking. Growth of a bony lump (exostosis) at the side of the big toe joint. Irritated skin around the bunion. Redness. Thickening of overlying skin. Blisters may form more easily. Deformed bones, joints and ligaments as the big toe shifts towards the other toes. As the big toe shifts, its base becomes more prominent, forming the bunion. Eventually the big toe is forced to lie over, or more commonly under, the second toe. The second toe of patients who have bunions commonly forms a hammer toe. Trouble with shoes. It is difficult to find shoes that fit properly. Bunions may force you to buy a larger size shoe to accommodate the width the bunion creates. Eventually it hurts to wear any shoe, or even walk barefoot. Diagnosis People with bunions may be concerned about the changing appearance of their feet, but it is usually the pain caused by the condition that leads them to consult their doctor. The doctor will evaluate any symptoms experienced and examine the affected foot for joint enlargement, tissue swelling and/or tenderness. They will also assess any risk factors for the condition and will ask about family history. An x-ray of the foot is usually recommended so that the alignment of big toe joint can be assessed. This would also allow any other conditions that may be affecting the joint, such as arthritis, to be seen. Non Surgical Treatment Except in severe cases, treatment for bunions is usually given to first relieve the pain and pressure, and then to stop the bunion from growing. Conservative treatment for bunions may include protective padding, typically with felt material, to prevent friction and reduce inflammation. Removing corns and calluses, which contribute to irritation. Precisely fitted footwear that?s designed to accommodate the existing bunion. Orthotic devices to stabilize the joint and correctly position the foot for walking and standing. Exercises to prevent stiffness and encourage joint mobility. Nighttime splints that help align the toes and joint properly. In some cases, conservative treatment might not be able to prevent further damage. This depends on the size of the bunion, the degree of misalignment, and the amount of pain experienced. Bunion surgery, called a bunionectomy, may be recommended in severe cases. This surgery removes the bunion and realigns the toe. 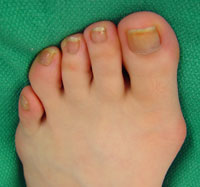 Surgical Treatment The most significant portion of the bunion surgery is re-aligning the bones. This is performed though bone cuts or a fusion involving the first metatarsal. The severity of the bunion determines where the bone will be cut or fused. Mild or moderate bunions can be corrected close to the big toe joint. Moderate or large bunions often require that the bone work be performed further away from the big toe joint to swing the bone in the proper position.
A patient recently came in with pain on the bottom of her right foot. The pain started several days after a night of dancing. She was not doing anything crazy, simply dancing for a few hours with frequent breaks standing at a table.
There you have it - wearing stilettos or high-heeled shoes for long periods of time can result in foot and ankle problems that include , heel pain, and painful trapped nerves. Cramming toes into narrow pointed-toe shoes can cause corns, calluses and toe deformities.  The presence of high uric acid level in the blood or the hyperuricemia is yet another certainty with the gout foot symptoms. Sometimes, tophi can come out. Tophi is a serious condition. Tophi or the uric acid build crystals under the skin can be seen as a symptom with the gout foot problems. Usually tophi can be seen near the Halux Valgus area. Gout attack along the foot can be recurrent. However, the frequency of the recurrent foot attack can vary upon the treatment and the proper food diet. Sometimes the gout attack can come back after few months or sometimes it can come back after a year or so. Listerine mouth wash is also very effective for treating toe nail fungus. Keep your toes in Listerine mouthwash. Your nails will healthier due to its powerful antiseptic leaves. Heels are usually worn out to fancy places such as restaurants or bars. They are also worn at weddings and anything formal like that. Many women wear high heels to work to feel professional and show off a great little shoe. High heels can also be worn under dress pants or with a skirt to wear just about anywhere that you can imagine, as long as you are comfortable and do not have to do any running. There are sensible precautions that you can take which allow you to continue wearing womens heels with minimal to no Foot Pain. Wear womens heels that are two inches or less. Womens heels disrupt gait and posture for the entire body. Shoes For Women that are greater than two inches significantly influence lower extremity mechanics and gait. Stretching the calf muscles will reduce some of the tension and tightness in the Achilles tendon and plantar fascia. Plantar fasciitis and calcaneal bursitis are common among runway models and ballroom dancers. Be picky about your shoes. Make sure you get shoes with firm heels that support and stabilize. There should be plenty of room for your toes. Break news shoe in gradually, only an hour or two at a time. The last but not least, you should choose shoes that can make your feet comfortable when ou are walking. More often, you should choose the shoes which can have half an inch of space left when you try on them. If you are going to buy heel shoes, you had better select the one that has proper heel height so that your feet will not feel painful when you are walking. |
AuthorWrite something about yourself. No need to be fancy, just an overview. Archives
July 2017
Categories |
 RSS Feed
RSS Feed
